Not long ago, a newfound friend of mine had shed light on the challenges medical billing professionals are facing.
They are severely outdated, still filling out forms in longhand, she cried. Faxes are still in use, pen and paper. The high churn rate of personnel and onboarding new trainees steal precious time. A myriad of errors ensues from that hindrance. It sounded to me like inefficiency hell, and it rang a great loss of money.
She’s been in the healthcare industry for over 20 years and has seen it all. Can we do something?
Disorganization, when coupled with inability and incapability will severely damage cash-flow and profitability. The more efficient and productive your business is, the more money it generates. More importantly, the profit left in your pocket is bigger, because working with tight workforce lowers your costs.
Now, at the time, I wasn’t an expert on Revenue Cycle Management, she was. I’m not “the expert” on Revenue Cycle Management, yet, (somewhat of a specialist). I am however “the expert” on increasing office productivity and efficiency. A facilitator who’s best at finding the easiest way to transform any workplace into a lean, unerring, money-making machine.
How do we improve our revenue cycle management?
First, we need to understand…
HOW REVENUE CYCLE MANAGEMENT WORKS
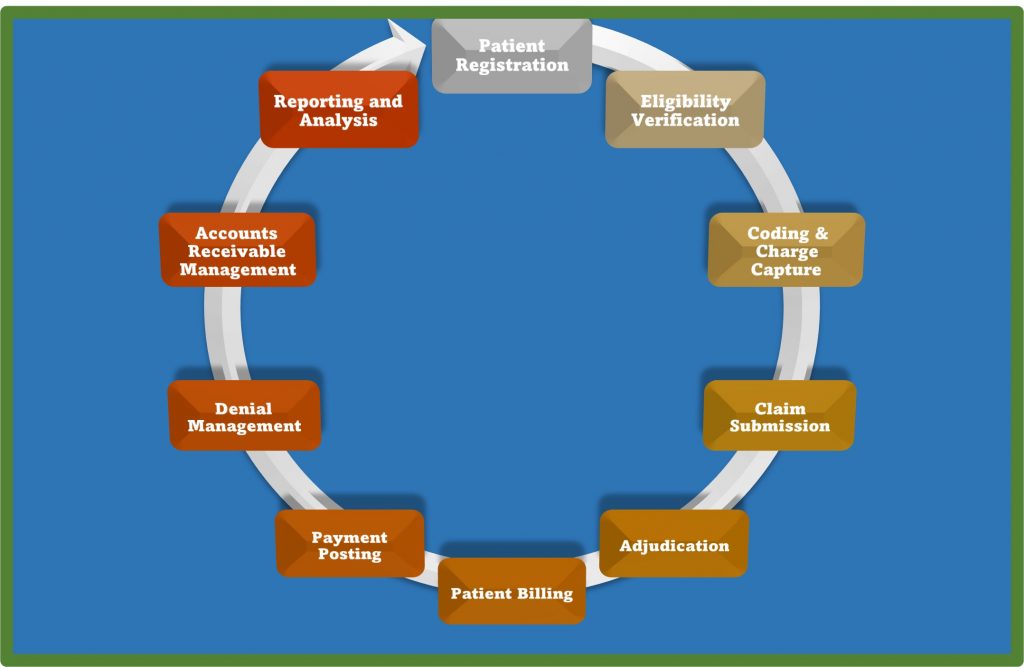
Healthcare providers, from hospitals to clinics, rely on a well-organized revenue cycle to ensure the financial health of their institutions. Let’s delve into the key components that make up this intricate process.
Patient Registration:
The revenue cycle begins with patient registration. Accurate and detailed information must be collected, including demographic details, insurance information, and any relevant medical history.
This step sets the foundation for interactions and billing processes. It must be accurate and quick. The data collected must be able to automatically fill out designated forms in order to achieve the elusive goal of labor-saving workplace.
Eligibility Verification:
Before providing services, it’s essential to verify the patient’s insurance eligibility. This step helps prevent claim denials and ensures that services rendered are covered by the patient’s insurance plan.
Coding and Charge Capture:
Once services are provided, billers and coders document the procedures and diagnoses using standardized codes (ICD-10 and CPT codes). Accurate coding is vital, as it directly influences reimbursement rates and claim approvals. The faster you process the forms, the faster you get paid.
In the ever-evolving landscape of healthcare:
- The NUCC (National Uniform Claim Committee) 1500 health insurance claim instruction manual is posted with new codes and procedures yearly in July.
- Ever-changing HCPCS, CPT, and ICM codes are something to take into account and prepare for.
- Fast evolving OCR (Optical Character Recognition) technology, capturing errors such as small as punctuation.
These are just a few challenges your Personnel and new trainees need to tackle while calculating claim amounts.
Claim Submission:
The coded information is used to generate claims, which are submitted to insurance payers for reimbursement. Timely and accurate claim submission is critical to prevent delays in receiving payments.
Adjudication:
After claim submission, insurance companies review and process the claims. This involves assessing the claim for accuracy, determining coverage, and calculating the amount payable. This step may result in partial or full claim denial. Denials must be documented, recorded, and analyzed to make sure mistakes do not repeat themselves repeatedly.
Patient Billing:
Once the insurance payer processes the claim, any remaining balance is billed to the patient. Clear and transparent patient billing statements facilitate prompt payment and reduce the risk of unpaid accounts.
Payment Posting:
Payments received from both insurance companies and patients are recorded and posted to the patient’s account. This step ensures accurate financial tracking and helps identify outstanding balances.
Denial Management:
Claims may be denied for various reasons, such as incomplete information or lack of medical necessity. An effective denial management process involves investigating and appealing denied claims to maximize reimbursement.
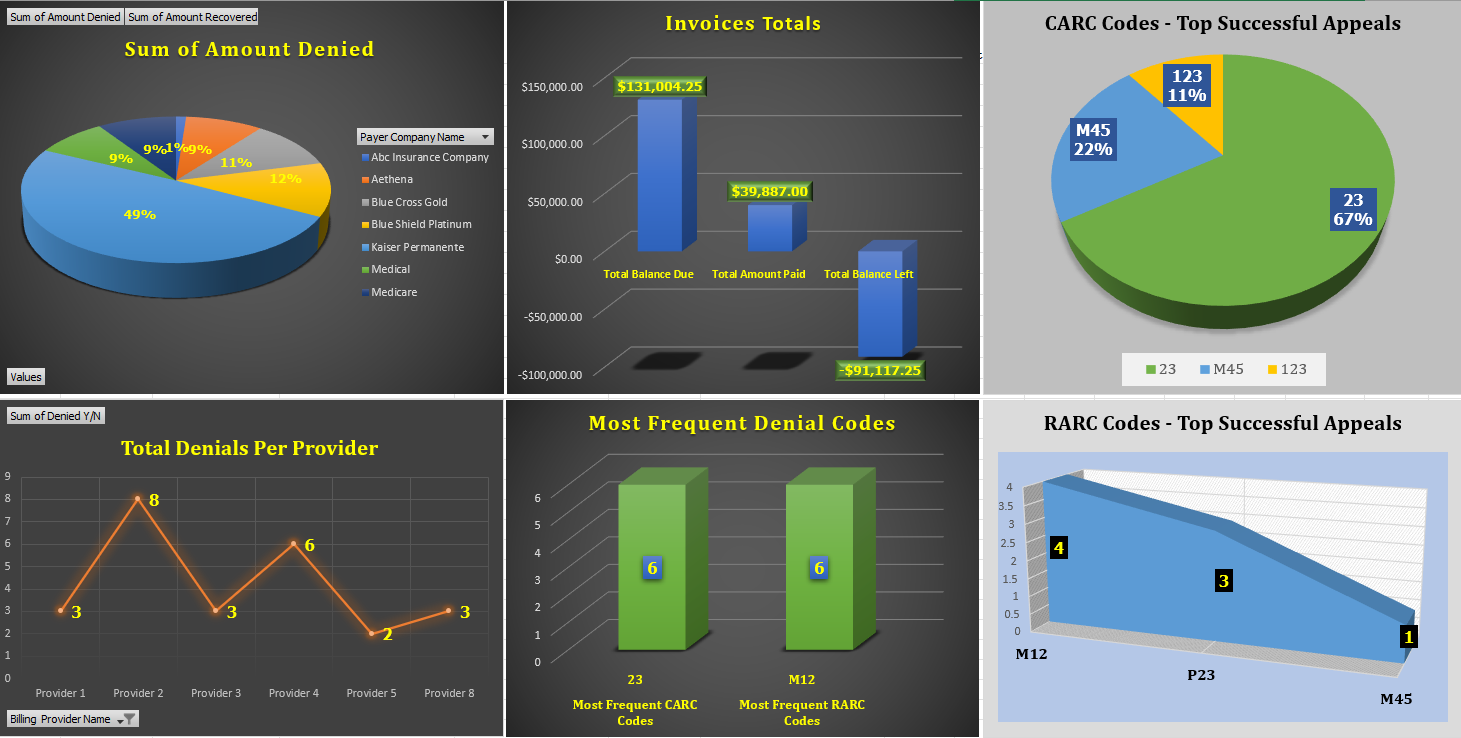
Controlling and analyzing your denials is the most crucial stage. Losing track of your denials results in losing money.
Accounts Receivable Management:
Monitoring and managing accounts receivable is pivotal for maintaining a healthy cash-flow. Timely follow-up on outstanding payments and resolving discrepancies are the way you make money.
If you lose track of your accounts receivables, you hurt your cash-flow and efficiency. Your personnel need to stop what they’re doing and look for the missing account and money.
Reporting and Analysis:
Regular reporting and analysis of key performance indicators (KPIs) help healthcare organizations identify trends. It streamlines processes, and helps making informed decisions for continuous improvement in the revenue cycle.
Define and monitor key performance indicators to assess the efficiency of your RCM process. Metrics such as days in accounts receivable, claim denial rates, and first-pass resolution rates.
All provide valuable insights for continuous improvement. You need the knowledge, ability, and way to enter error-free data into those reports and conduct a constructive analysis of those reports.
STRATEGIES FOR STREAMLINING YOUR REVENUE CYCLE MANAGEMENT PROCESS
There are key strategies that can enhance revenue cycle and navigate the complexities of financial management successfully:
The Patient-Centric Approach:
Educate patients about their financial responsibility upfront. Provide clear explanations of co-pays, deductibles, and any out-of-pocket expenses. Transparent communication enhances patient satisfaction and reduces billing-related inquiries. This can be done via brochures, emails, text links, and other material that can be sent to patients before entering your office.
Streamlined Patient Registration:
Implement robust registration processes to capture accurate patient information, insurance details, and demographic data. This reduces billing errors and ensures a smoother billing workflow.
Insurance Verification:
Conduct real-time insurance eligibility checks to confirm coverage details before services are rendered. This helps prevent claim denials due to insurance-related issues. Accurate patient data is foundational.
Implement robust systems for capturing all data and verifying insurance coverage, eligibility, and demographic details. This proactive approach minimizes claim rejections and accelerates the reimbursement process.
Effective Coding and Documentation:
Ensure accurate and detailed coding of medical services. Regularly train staff on coding updates and changes to avoid coding errors that could lead to claim denials or delays.
Prompt Claim Submission:
Leverage technology to submit claims electronically and monitor claim statuses for any discrepancies.
Automated Billing Systems:
Implement advanced billing software that automates billing processes, reducing the risk of errors and expediting the revenue cycle. Automation enhances efficiency, allowing staff to focus on more complex tasks.
Regular Financial Audits:
Conduct regular audits of your financial processes to identify and rectify any discrepancies promptly. This proactive approach can prevent revenue leakage and ensure compliance with industry standards.
Strategic Denial Management:
Develop a comprehensive denial management strategy to identify patterns, address root causes, and appeal denials effectively. This proactive approach can significantly reduce revenue loss.
Patient Payment Portals:
Offer online payment options and patient portals to facilitate easy and secure payment transactions. This not only enhances the patient’s experience but also accelerates revenue collection.
Staff Training and Education:
Minimize the time invested in continuous training. Keep your billing and administrative staff abreast of the latest industry regulations, coding updates, and best practices. Utilize the correct software that will take away the need from new trainees to master everything, and will guide them into the making correct choices.
THE ROLE OF TECHNOLOGY IN IMPROVING REVENUE CYCLE MANAGEMENT
Streamlining the billing process not only ensures timely payments but also reduces the risk of errors and denials. Here are key strategies to optimize your RCM and enhance overall efficiency.
Invest in Technology:
Embrace advanced billing software and electronic health record (EHR) systems. Automation can significantly reduce manual errors, enhance coding accuracy, and expedite claims processing.
The key takeaway is invest not buy or pay, but make an investment in the right program that will best fit your organization. A program that will not only save you money, but make you money by enabling your team to process more claims. A program that could control claim management and account receivables. Your investment will be paid off very fast and your Return on Investment will be unparalleled.
Effective Documentation:
Thorough and precise documentation is vital for successful billing. Ensure that medical coders and providers collaborate effectively to capture all relevant information. This not only prevents billing discrepancies but also supports better communication with payers.
Claim Scrubbing:
Integrate a robust claim scrubbing system into your billing process. This technology identifies errors before claims are submitted, reducing the chances of rejections and denials.
Timely Submission of Claims:
Submit claims promptly to avoid delays in reimbursement. Develop a schedule for regular claim submissions, ensuring compliance with payer deadlines. Timeliness not only expedites revenue but also minimizes the risk of lost or forgotten claims.
Effective Communication:
Foster open communication channels with payers to resolve issues promptly. Regularly follow up on outstanding claims and establish clear protocols for handling denials. Proactive communication can lead to quicker dispute resolution and payment.
Regular Audits:
Conduct regular internal audits to identify areas for improvement. These audits can help identify patterns of errors, address root causes, and implement preventive measures, ultimately leading to a more streamlined revenue cycle.
HOW AUTOMATING YOUR REVENUE CYCLE CAN INCREASE EFFICIENCY
Manual medical billing processes can be time-consuming, error-prone, and hinder overall efficiency. Embracing automation in your revenue cycle can bring about transformative benefits.
Streamlined Billing Processes:
Automating medical billing tasks minimizes the risk of human error and ensures accurate and timely submissions. This streamlining of processes reduces the likelihood of claim denials. It allows your organization to receive payments faster and maintain a healthier cash flow.
Enhanced Claim Accuracy:
Automated systems use advanced algorithms to cross-verify patient data, insurance information, and coding accuracy. This significantly reduces the chances of errors that might lead to claim rejections. By improving claim accuracy, you not only save time but also enhance the overall reimbursement process.
Faster Reimbursements:
Automated systems expedite the claims processing cycle, reducing the time it takes for reimbursements. Timely submission of clean claims results in quicker payments, positively impacting your organization’s financial health. This efficiency is especially crucial in the current healthcare landscape where providers face increasing financial pressures.
Improved Patient Experience:
Automation extends beyond the back-end processes and can positively impact the patient experience. By expediting billing and reimbursement, patients receive clear and accurate statements, leading to improved satisfaction. This, in turn, contributes to better patient-provider relationships and can positively influence patient retention.
Compliance and Auditing:
Automated systems can incorporate compliance checks and audit trails, ensuring that your billing practices adhere to ever-evolving healthcare regulations. This not only reduces the risk of penalties but also provides a transparent record of financial transactions, fostering accountability and integrity.
Resource Optimization:
With automation handling repetitive tasks, your staff can focus on more value-added activities, such as patient care and strategic planning. This leads to a more efficient allocation of resources, boosting overall productivity within the organization.
Adaptability to Industry Changes:
The healthcare landscape is dynamic, with frequent changes in regulations, coding standards, and payer requirements. Automated systems can be updated swiftly to adapt to these changes, ensuring ongoing compliance and reducing the burden of manual updates on your team.
THE IMPACT OF AUTOMATION ON REVENUE CYCLE PERFORMANCE
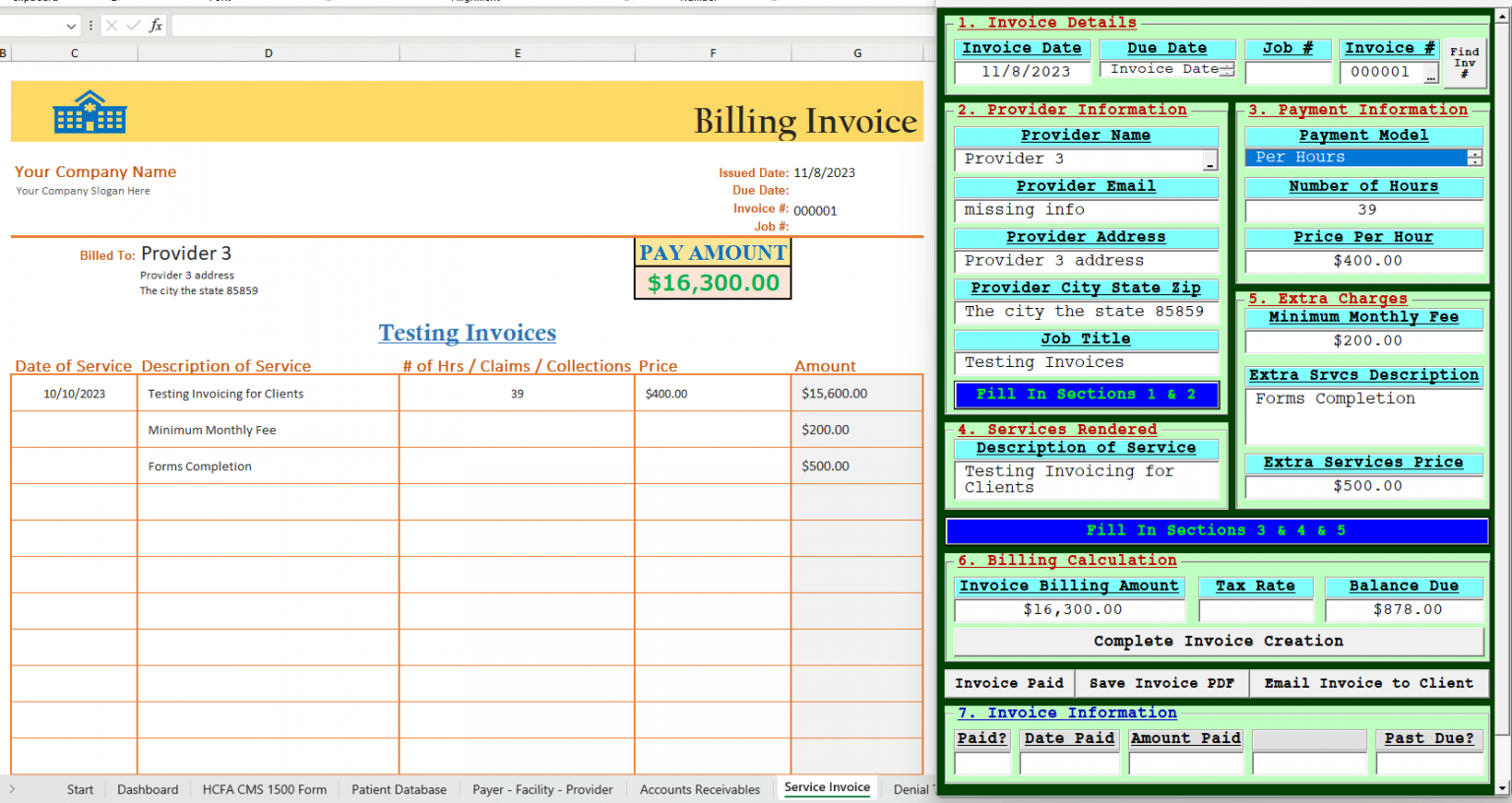
Time saving. Cost-effective. Errorfree. All emanate from the ability to create new invoices instantly and capture all imperative data in an account receivables database as claim complete.
The ability to reduce paperwork and fill out the least amount of forms possible in a systematic and economical way is key factor in achieving profitability.
Your best bet would be a custom-made software that is created solely on implementing the right strategy. One that fits your business and staff’s savviness. A program that suits your way of doing business and running operations.
One that blends with your autogenic (self-produced) forms, and your self-made database. It will help you revamp your office and modernize your systems. It’ll make your revenue cycle management easier, trackable, analysis-prone, and error-free.
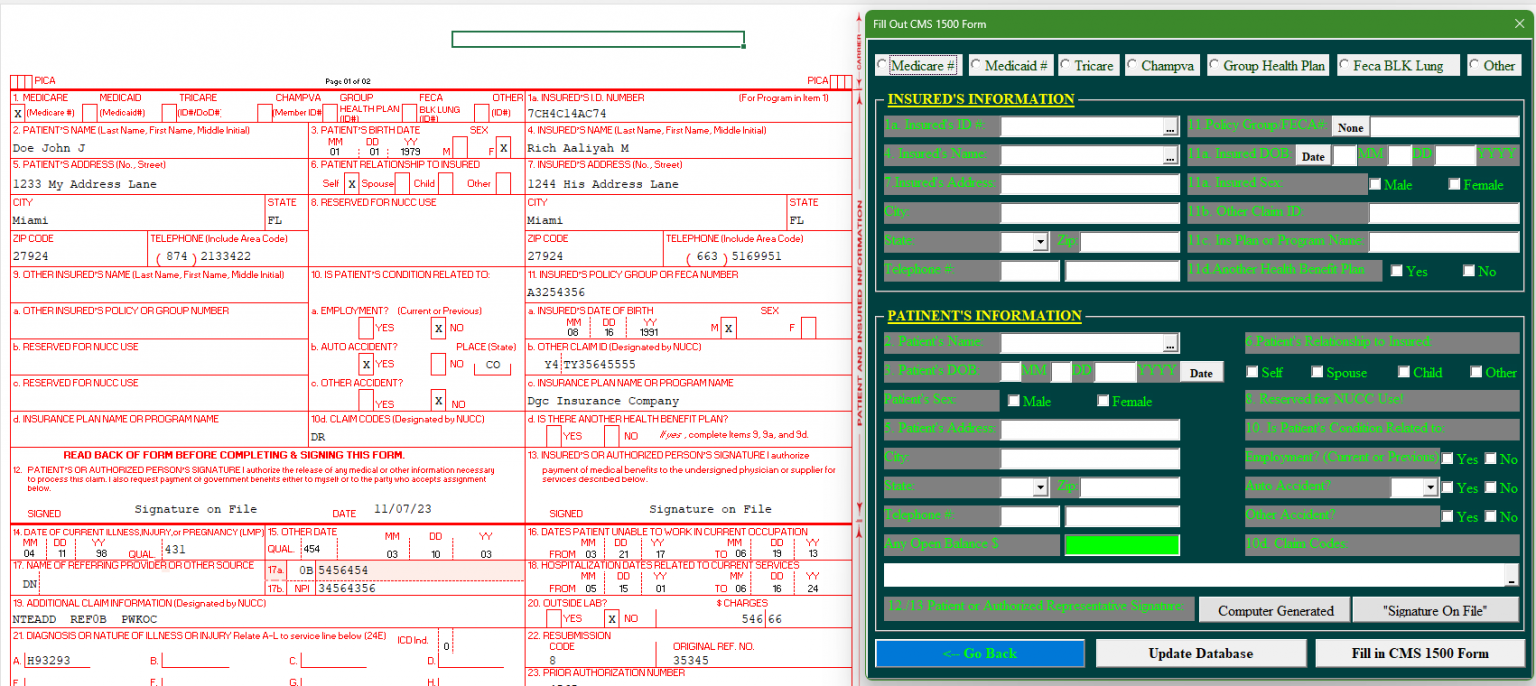
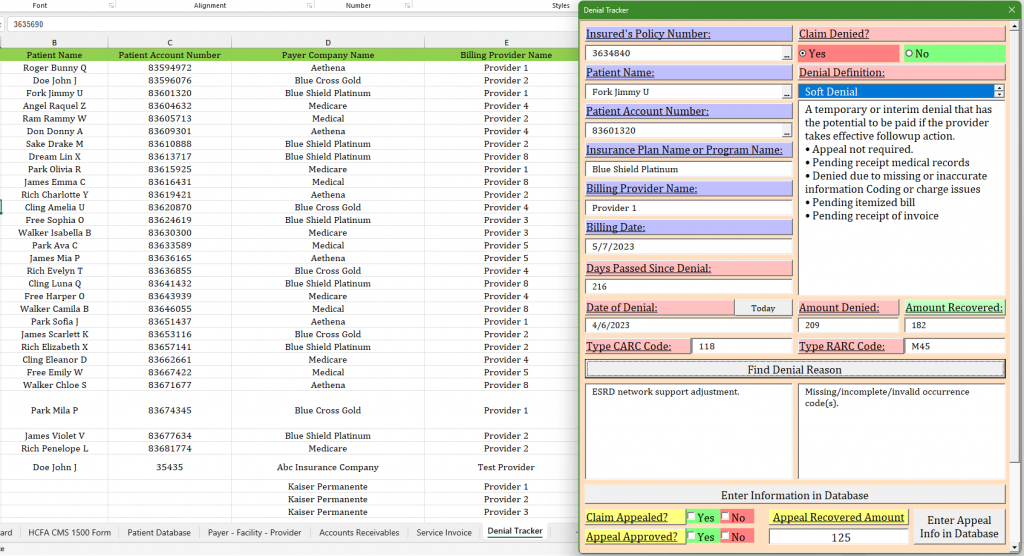
One crucial tool that plays a pivotal role in this process is a CMS-1500 software.
CMS-1500 is the standard claim form used by healthcare providers to submit bills for reimbursement. It serves as the primary vehicle for communicating patient information, diagnosis, and treatment details to insurance payers.
To streamline this intricate process, CMS-1500 software emerges as a valuable ally, offering a range of features that enhance accuracy and efficiency.
Key Features of CMS-1500 Software:
Data Accuracy:
CMS-1500 software minimizes the risk of errors by providing structured fields for entering patient information, ensuring accuracy in billing details.
Claim Submission:
Electronic submission of claims is a hallmark feature, expediting the billing process and reducing the time it takes to receive reimbursements.
Code Integration:
Integration with medical coding systems facilitates the inclusion of accurate procedure and diagnosis codes, eliminating discrepancies and potential claim denials.
Customizable Templates:
Providers can create customizable templates based on the type of services offered, reducing the time spent on repetitive data entry.
Time Efficiency:
CMS-1500 software accelerates the billing process, allowing healthcare providers to focus more on patient care and less on administrative tasks.
Reduced Errors:
The structured format of the CMS-1500 form, coupled with validation checks in the software, helps reduce errors in billing, minimizing the chances of claim denials.
Improved Cash Flow:
Quicker claim submission and processing translate to faster reimbursement, contributing to improved cash flow for healthcare practices.
Compliance Adherence:
The software ensures that claims adhere to the latest regulatory requirements, promoting compliance and reducing the risk of audits.
IN CONCLUSION...
When selecting CMS-1500 software, healthcare providers should consider these crucial key factors:
- User-friendliness.
- Integration capabilities with existing systems.
- Customizability to fit your business needs.
- Adding reports as you go.
- Adding new functionalities as needed.
- Adding new forms as needed.
- Generating a database from the first stage of patient registration and then on.
- Regular code updates.
- Responsive customer support.
Optimizing RCM is a critical step toward long-term success. By implementing the right strategies and software, healthcare organizations can fortify their revenue cycle management. They can minimize errors, and ensure a more efficient billing process, thus ensuring financial stability and sustainability.
As the industry continues to evolve, embracing automation becomes not only a competitive advantage but a necessary step in ensuring long-term financial viability and exceptional patient care.
CMS-1500 software stands as a cornerstone in the healthcare billing landscape. It offers providers a reliable and efficient solution for navigating the complexities of medical billing.

Author
Asaf Antman is a pioneer of the alternative lending industry with more than two decades of extensive experience in the business world under his belt. Throughout his career, he dissected thousands of businesses; underwrote, analyzed, advised, negotiated debts, secured deals, and funded small to mid-size companies in a variety of industries and locations across the U.S.